(10-minute read)
Quick Navigation – Click the links below to jump to that section of the info-brief or continuing scrolling to read the brief in its entirety.
Fentanyl is driving the overdose rate throughout the United States
Substances seized by law enforcement mirror substances causing overdose deaths
What is nonpharmaceutical fentanyl?
Why is nonpharmaceutical fentanyl in the drug supply?
Why are fentanyl overdoses occurring?
How is the State of Maine actively responding to the fentanyl epidemic?
Fentanyl is driving the overdose epidemic both nationally and in the State of Maine
Both nationally and in the State of Maine, nonfatal and fatal drug overdoses are being driven higher by the lethality of co-intoxicants in the drug supply. The most notable of these is nonpharmaceutical fentanyl and its analogs such as acetylfentanyl, furanylfentanyl, and carfentanil. Seen in the charts below, the abrupt rise in drug deaths beginning in 2014 corresponds to the increase of fentanyl in the toxicology of decedents both in Maine and across the United States. The rise and fall of Maine drug death numbers mirror national trends with a peak in 2017 followed by a dip in 2018 and a sharp rise beginning in 2019 and continuing through 2021.
Source: Maine Drug Data Hub, Monthly Overdose Report; Drug overdose deaths in the United States, 1999–2020. NCHS Data Brief, no 428.
Note: Natural and semi-synthetic opioids include pharmaceutical drugs such as morphine, oxycodone, and hydrocodone. Synthetic opioids do not include methadone. Synthetic opioids include drugs such as fentanyl, fentanyl analogs, and nonpharmaceutical tramadol.
As seen above, synthetic opioid/fentanyl overdoses began increasing in 2013 leading to nearly exponential growth beginning in 2014. In 2017, all fatal opioid overdoses in the United States and all fatal drug overdoses and fatal fentanyl overdoses in Maine peaked then dipped slightly in 2018. In 2019, fatal overdoses rose again and reached the grim milestone of 100,000 deaths in the United States between March 2020 to April 2021. In Maine drug deaths increased 7% in 2019, 36% in 2020, and an estimated 23% in 2021. During this time, drug deaths and nonfatal overdoses have also increased due in part to the global covid-19 pandemic. Below is a graph that highlights the percentage of drug deaths in Maine where fentanyl listed as a cause of death.
Source: Rural Drug and Alcohol Research Team, Margaret Chase Smith Policy Center, University of Maine.
The substances seized by law enforcement in the illicit drug supply mirrors overdose deaths
Below, the same pattern of fatal drug overdoses by substance is seen in the grams of drugs seized by Maine DEA task forces and the pounds of drugs seized by Customs and Border Protection (CBP). This indicates that fatal drug overdoses are related to the lethality and potency of substances in the illicit drug supply. MDEA heroin seizures peaked in 2019 dropping in 2020 and 2021. This same pattern is replicated in the CBP drug seizures nationally. Seizures of pharmaceutical drugs peaked in 2019 and also dramatically dropped in 2020 and 2021. Fentanyl seizures, much like drug deaths, peaked in 2017 dipped in 2018, and abruptly rose beginning in 2019 and continues through 2021. CBP drug seizures saw fentanyl sharply rise from 2017 to the present. In both MDEA and CBP data methamphetamine began sharply rising in 2018.
Source: Maine Drug Data Hub Prevention Metrics; U.S. Customers and Border Protection CBP Enforcement Statistics. Note, CBP fentanyl seizures listed as N/A prior to 2017.
What is nonpharmaceutical fentanyl?
Nonpharmaceutical fentanyl and its analogs are synthetic opioids typically manufactured in China and shipped to drug cartels in Mexico for distribution throughout the United States. They are significantly more potent than other opioids—including oxycodone and heroin—however, the purity and concentrations of fentanyl is unknown to users both in their total supply or in their individual doses. Fentanyl is up to 25 times more potent than oxycodone and 50-100 times more potent than heroin. Some fentanyl analogs, such as carfentanil, are 100 times more potent than nonpharmaceutical fentanyl. Despite its potency, naloxone is still an effective medication that can potentially reverse an opioid overdose caused by fentanyl and its analogs if quickly administered by bystanders or public safety personnel. That is why it is important to #haveitonhand.
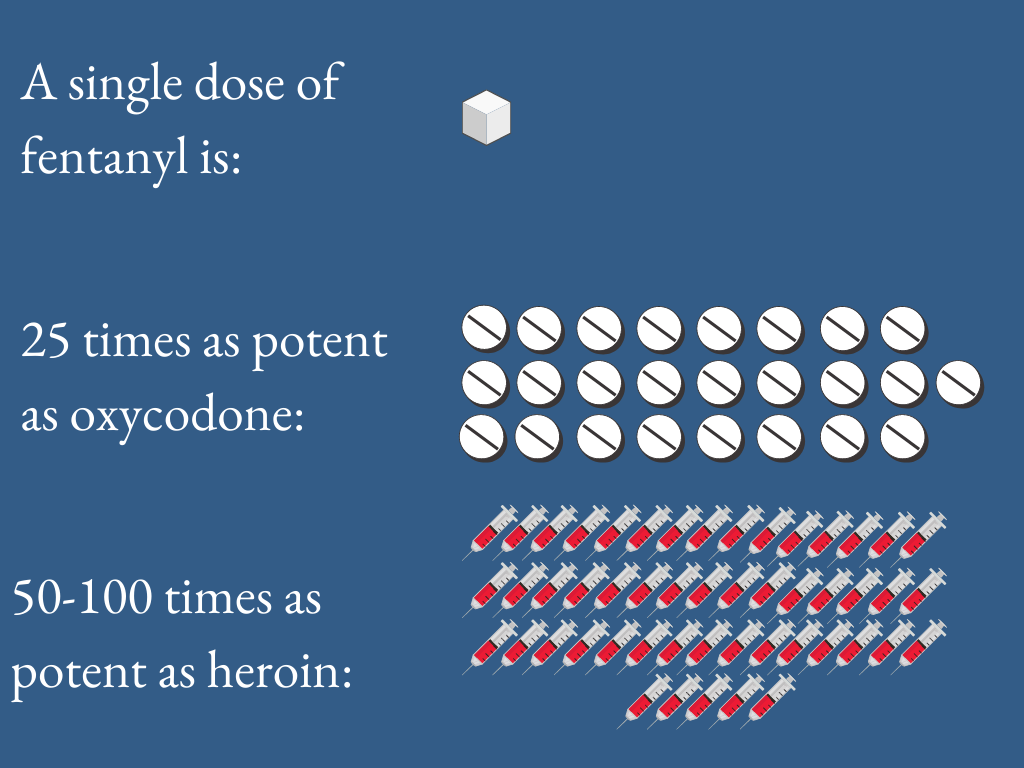
Why is nonpharmaceutical fentanyl in the illicit drug supply?
Nonpharmaceutical fentanyl and its analogs are in the drug supply because it is cheaper and easier to create the chemical compounds needed to manufacture these synthetic opioids than it is to grow opium poppy plants and manufacture heroin from morphine. Fentanyl and its analogs also have a much greater potency than heroin and produce a much greater yield per kilogram than any other opioids. Heroin, by contrast, is a heavy and bulky product making it more difficult to ship and conceal during illicit distribution.
Fentanyl is frequently added to other opioids such as heroin. However, it is also added to stimulants such as cocaine and methamphetamine and other illicitly purchased substances such as marijuana and ecstasy/Molly (MDMA) to produce novel effects. This often occurs without the users’ knowledge. By adding even small amounts of fentanyl to a less potent drug, producers, dealers, and consumers can stretch their drug supply and increase their profits.

Why are fentanyl overdoses occurring?
As mentioned above, fentanyl and its analogs are more lethal than pharmaceutical opioids and other illicit opioids, such as heroin, due to their potency as well as the unknown purity and concentrations in the illicit drug supply or in individuals doses. In some death investigations, users are found to have experienced a fentanyl overdose before the syringe is removed. That is why it is essential for bystanders to carry naloxone, call 9-1-1 in the event of an emergency, and understand how to respond to an opioid overdose. It is also essential that individuals to never use alone.
In addition to opioid users, stimulant users and persons using illicit street pharmaceuticals and marijuana unknowingly have consumed fentanyl and overdosed due to their supply being adulterated by these powerful synthetic opioids. Even for stimulant and psychedelic users, naloxone should be carried by bystanders and individuals should never use alone.
Source: Rural Drug and Alcohol Research Team, Margaret Chase Smith Policy Center, University of Maine.
As seen above, the drug deaths involving combinations of fentanyl with other illicit substances have been trending upwards over the past nine years. Fatal overdoses in Maine involving fentanyl and other key illicit substances mirror MDEA and Customs and Border Protection drug seizures with fentanyl related overdoses increasing dramatically in 2017 and methamphetamine related overdoses increasing nearly exponentially from 2018 to 2021. Additionally, since 2018 overdoses involving heroin have been decreasing corresponding with decreasing seizures of the drug both in Maine and nationally beginning in 2019 and continuing through the present.
How is the State of Maine actively responding to this epidemic of fentanyl overdoses?
Though the State of Maine is engaged in many novel and evidence-based substance-use disorder programs, the following harm reduction and investigative programs are currently, or have the potential to, save victims of the fentanyl epidemic in Maine.
Office of the Maine Attorney General Naloxone Administration Program
Beginning in 2016, the Office of the Maine Attorney General began distributing naloxone to law enforcement officers to administer to overdose victims and save lives in the communities that they serve. Beginning in August of 2019, law enforcement officers also began reporting nonfatal overdoses they respond to in OD MAP—an overdose mapping software designed to identify geospatial spikes and patterns in overdoses for public health and public safety response. Nonfatal overdose responses by law enforcement officers is a measure of individuals who were revived during an overdose emergency by public safety personnel. Over the past 6 years, 911 opioid overdose reversals have been reported by law enforcement personnel.
Source: Maine Naloxone Distribution Initiative, Margaret Chase Smith Policy Center, University of Maine. OD MAP and OAG naloxone overdose responses deduplicated.
Maine Naloxone Distribution Initiative
Since 2019, the State of Maine has made State-supplied naloxone available to organizations and members of the community that wish to have-it-on-hand in case of an opioid overdose emergency or to distribute to individuals that use opioids as well as their loved ones. During its first two years, from July 2019 to July 2021, the Maine Naloxone Distribution Initiative and the Maine Attorney General’s Naloxone Distribution Program has distributed over 110,000 doses of naloxone to communities throughout Maine. These doses of naloxone have directly contributed to the successful reversal of 3,378 overdoses as reported to Maine Naloxone Distribution Initiative community partners as of December 2021.
Source: Maine Naloxone Distribution Initiative, Margaret Chase Smith Policy Center, University of Maine
The Overdose Prevention Through Intensive Outreach Naloxone and Safety (OPTIONS) initiative
The Overdose Prevention Through Intensive Outreach Naloxone and Safety (OPTIONS) initiative (https://knowyouroptions.me) aims to improve the health of Mainers using substances through harm reduction strategies, helping them on the road to recovery, and dramatically reducing the number of fatal and nonfatal overdose deaths.
The OPTIONS liaison initiative embeds licensed behavioral health clinicians within local emergency medical services (EMS) and law enforcement agencies in every county across Maine. Liaisons work alongside their first responder counterparts to:
- Engage in post-overdose followup and help with referrals.
- Conduct proactive outreach with at-risk communities.
- De-escalate behavioral health crises when possible.
- Provide short-term counseling interventions when appropriate.
Each OPTIONS liaison serves the entire county in which they are located. As part of the OPTIONS liaison initiative, the Office of Behavioral Health and the Maine Center for Disease Control and Prevention are working to better integrate the varying levels of support services in each county. These services include Syringe Access Programs, naloxone distribution, Recovery Centers, medication for opioid-use disorder providers, food and housing support among others.
Source: Maine Naloxone Distribution Initiative, Margaret Chase Smith Policy Center, University of Maine. Co-response calls are when liaison respond to overdose and substance-use related emergencies alongside public safety. Post-overdose followup calls are when liaisons respond to overdoses reported to them by public safety or through OD MAP. Pro-active referrals are by affected others, treatment providers, public safety officials or others before an overdose has occurred. Self referrals are individuals who contact OPTIONS liaisons after learning about the programs from media campaigns, affected others, or some other means.
Source: Maine Naloxone Distribution Initiative, Margaret Chase Smith Policy Center, University of Maine. SUD Treatment is referrals to community-based treatment programs. Recovery referrals are to community-based recovery supports such as recovery community coalitions, recovery residences, or recovery centers. SSP referrals are to syringe service programs. Infectious disease referrals are for infectious disease testing such as HIV or Hepatitis C testing. MaineMOM referrals are for pregnant or postpartum persons to specialized services. For more information click here: MaineMOM website.
Source: Maine Naloxone Distribution Initiative, Margaret Chase Smith Policy Center, University of Maine. OPTIONS liaisons have distributed 909 kits of intranasal naloxone during its first year. 1 kit of intranasal naloxone contains two doses of medication. Training conducted by OPTIONS liaisons include overdose education and naloxone distribution trainings, anti-stigma trainings, substance use disorder education trainings, among others.
Overdose Review Panel
On June 21, 2021, Governor Mills signed into law L.D. 1718, An Act to Establish the Accidental Drug Overdose Death Review Panel. The law establishes an Accidental Drug Overdose Death Review Panel to review a subset of deaths caused by accidental drug overdoses and to recommend to state, county and local agencies methods of preventing deaths as the result of such overdoses, including modification or enactment of laws rules, policies and procedures. The panel is made of up fifteen (15) individuals representing a number of state offices, law enforcement agencies and including impacted family members and persons in recovery. The panel also will include one or more physicians who treat substance use disorder, an EMS representative and a harm reduction specialist. The panel is chaired by the state’s Director of Opioid Response and is staffed by the Rural Drug and Alcohol Research Team at the Margaret Chase Smith Policy Center at the University of Maine.
Source: This info-board was created by Jamie-Lynn Kane a graduate student research assistant at the Margaret Chase Smith Policy Center at the University of Maine with data and collaboration from the Rural Drug and Alcohol Research Program.